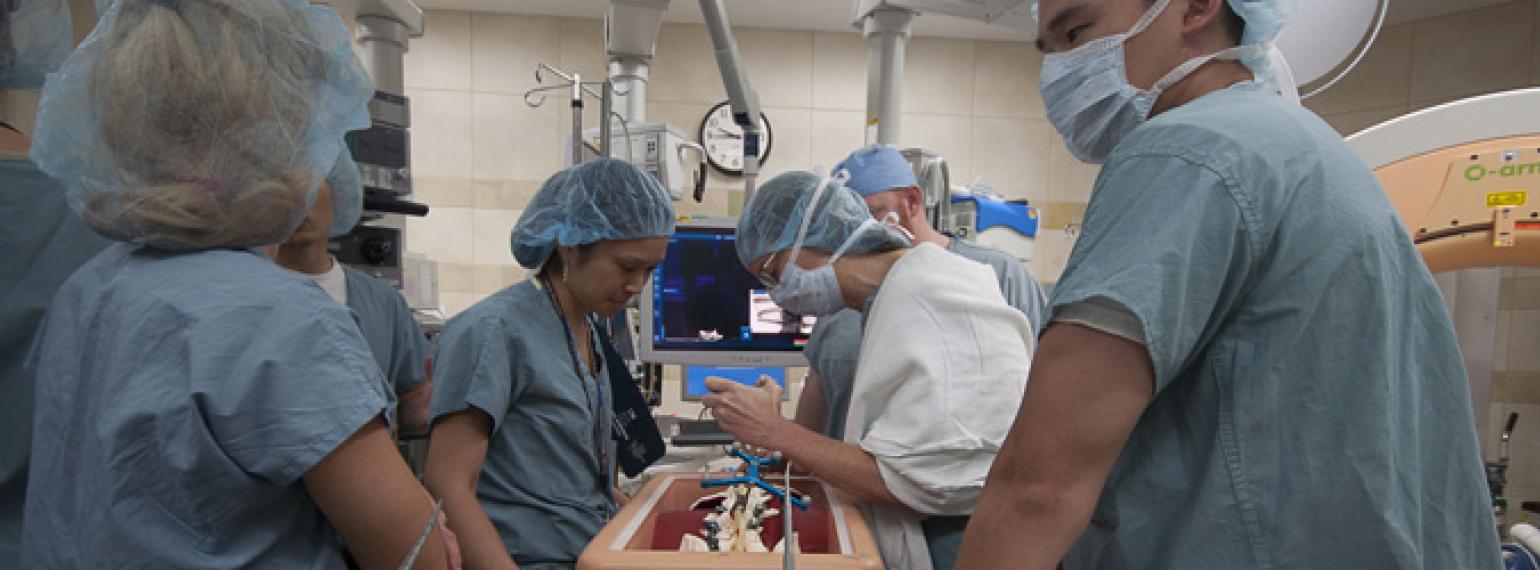
The faculty and staff of our department are dedicated to providing outstanding, state-of-the-art, evidence-based care for musculoskeletal injuries and conditions. Through our dedication to the interrelated missions of patient care, education, and research, we are able to provide the best and most appropriate care to each of our patients.
We believe that a multidisciplinary approach to musculoskeletal health, where bone and joint specialists with different backgrounds work together, provides optimal care for each individual patient. Our goal is to allow individuals to maintain a satisfying level of activity across their lifespan through the maintenance and restoration of musculoskeletal health and function.