Amongst the first of its kind, our training program is still one of the most sought-after in the country. Both our clinics and world-renowned research institute lead the industry in innovation and shape the future of patient care.

Every day, the U-M Medical School Department of Otolaryngology-Head & Neck Surgery is working to be the global leader in care, research and innovation. Our comprehensive adult and pediatric treatment of ear, nose, throat, head, and neck conditions include the country’s top center for laryngeal disorders, international fieldwork, and life-changing treatment within the University of Michigan hospital and clinics.
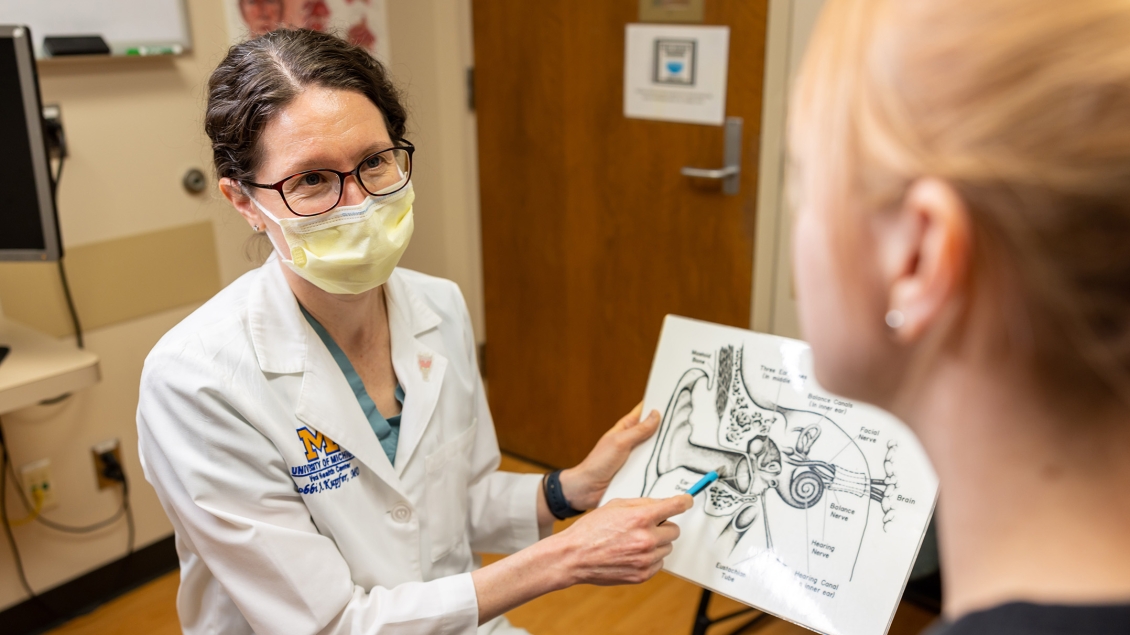
We provide patient care across a spectrum of focus areas and specialties within otolaryngology.
Since 1980, the department’s DEI committee has worked to create a safe space, combat racism, support health equity, and promote inclusion within the otolaryngology community.
Private support is the foundation of the vital work we do. From funding missions to treat patients in remote parts of the world, to saving the lives of babies and children with 3D printing, your gift is life-changing for patients, today and in generations to come.












Resources and information for current OTO learners and faculty.