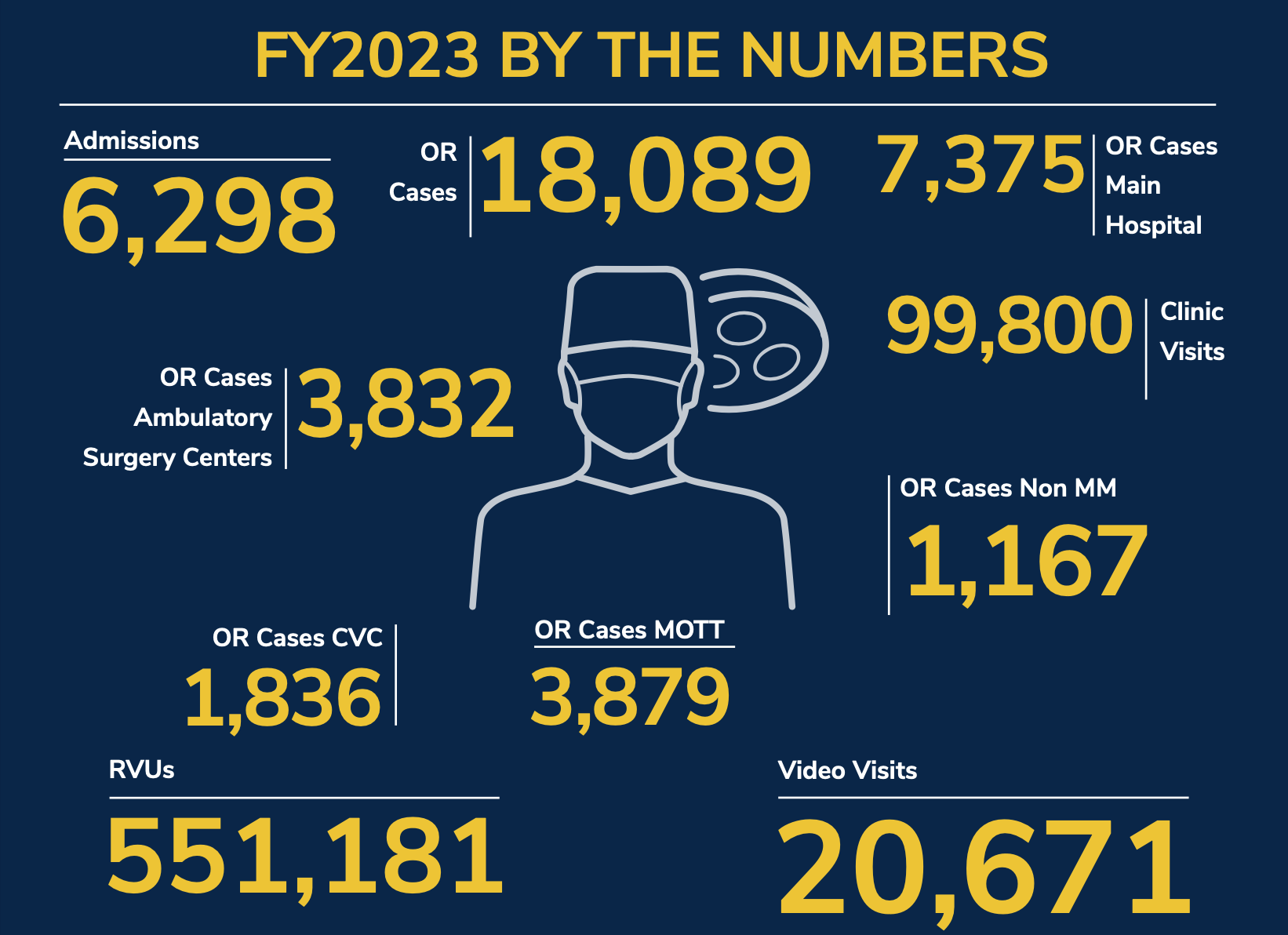
- 6,298 Admissions
- 18,089 Operating Room (OR) Cases: 7,375 Main Hospital; 3,832 Ambulatory Surgery Centers; 1,836 Cardiovascular Center; 3,879 C.S. Mott Children's Hospital; 1,167 Non-Michigan Medicine
- 99,800 Clinic Visits
- 551,181 RVUs
- 20,671 Video Visits
Each fall, we begin a new academic year at the University. It is a natural time for reflection and planning the year ahead. Two years ago, we were navigating the challenges of pandemic hospital surges yet were hopeful for some return to normalcy with the promise of vaccines.
We began to realize that promise last year, and set out to rebuild community with in-person events. I believe we made great progress in re-establishing a sense of community that the pandemic had eroded. I am energized by learning together in grand rounds, seminars and educational conferences. Rebuilding our interpersonal relationships is a source of renewal, and will continue to be an important goal over the course of this year.
Clinical Care: By the Numbers
Research: By the Numbers
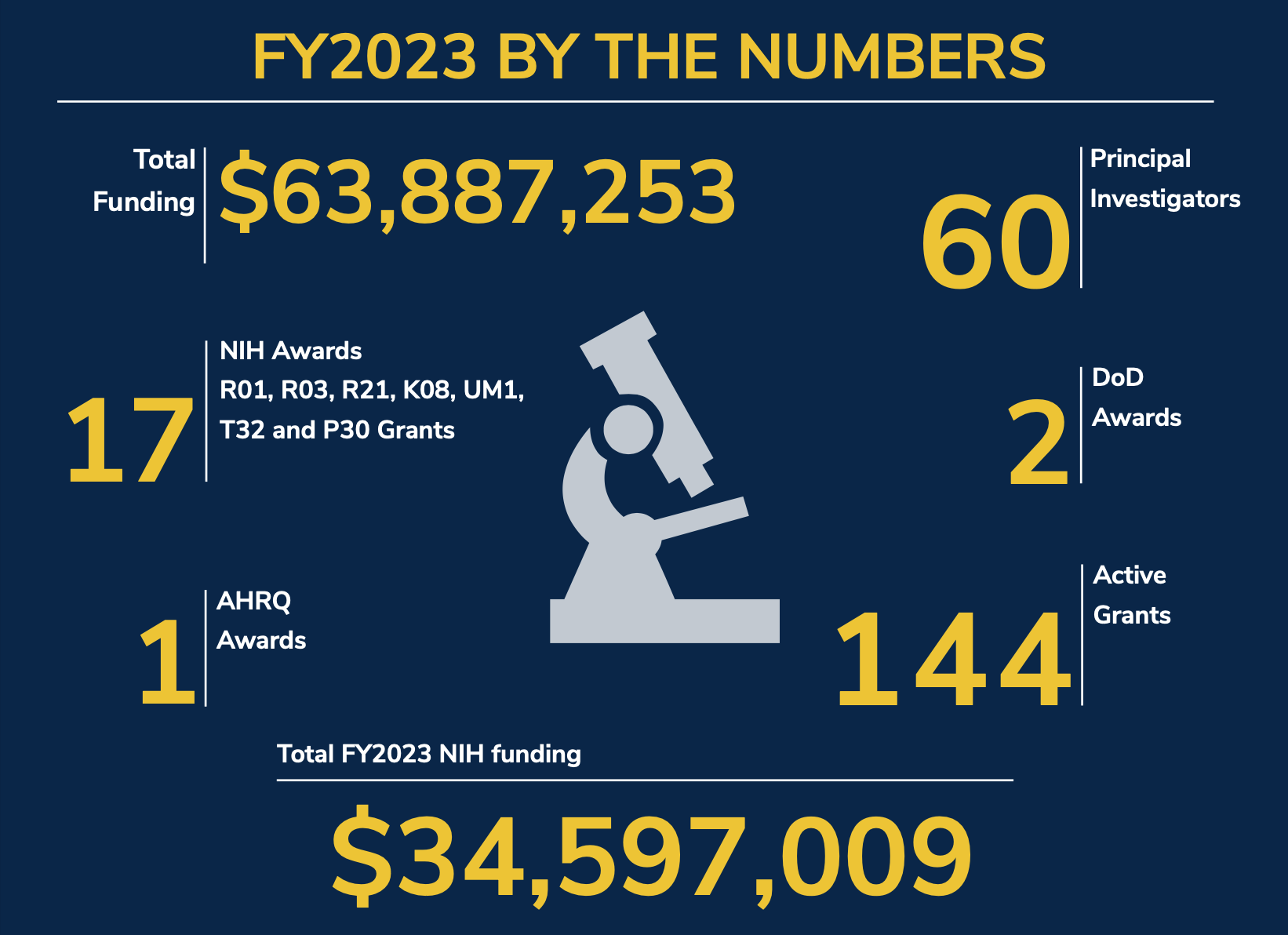

- $63,887,353 Total Funding
- 60 Principal Investigators
- 144 Active Grants
- 1 AHRQ Awards
- 2 Department of Defense Awards
- 17 NIH Awards (RO1, RO3, R21, K08, UM1, T32 and P30 Grants)
- $34,597,009 Total Fiscal Year 2023 NIH Funding
Education: By the Numbers

- 121 Residents: 80 Male, 72Female, 61 Underrepresented Minorities in Medicine, 28 Hold Advanced Degrees
- 3 T32 Grants
- 103 ACGME-Accredited House Officers
- 10 Residents Went on to a Fellowship
- 12 Residents Supported by T32
- 30 Fellows
Michigan Promise Highlights
Environment
We hosted the 5th Annual Asa Yancey lecture delivered by Dr. LJ Punch, Executive and Medical Director of the Bullet Related Injury Clinic in St. Louis, MO. His lecture was entitled “Black American Medicine: The Modern Legacy of Dr. Asa G. Yancey, Sr.” We also hosted Grand Rounds speakers on “Good Trouble: Surgeons as Advocates” delivered by Dr. Callisia Clarke, “Transplant Geography” delivered by Dr. Robert Cannon, and Dr. Mike Englesbe and Dr. Marina Pasca Di Magliano delivered presentations on their mini-sabbatical trips. Ten Cultural Complication sessions were hosted over the academic year, exploring topics such as “Managing Adverse Patient Outcomes,” “Medicalization of Size,” and “Mental Illness Among Providers.” Section gifts of healthy snacks and equipment were delivered to 11 surgery lounges across the Ann Arbor campus as an end-of-year gesture of appreciation. The Culture Crew hosted the annual Spring Retreat for faculty, staff, and APPs across sections.
Recruitment
Our 19-member recruitment committee participated in 34 group interview sessions to assist the Department in selecting the best candidates for open faculty positions during a busy recruitment season. We are excited to welcome 12 new faculty to the department this fall.
Achievement
We continued to support new faculty with our launch teams, which provide three years of team based leadership guided by a flexible curriculum of early-career development. A similar program for mid-career faculty, the Boost Team Program, is starting its third year, with three faculty in our current cohort. We also launched Accelerator teams, which are geared towards mid-career faculty who have taken on a new leadership role within our department.
Leadership
The Junior Faculty Exchange Program continued this past year with a full cohort. The department hosted 10 faculty over the course of the academic year and 10 of our own faculty visited other institutions. We held three additional professional development opportunities for the faculty, residents and learners in our department: the first Early Career Faculty Day, which focused on topics that help early career faculty succeed in all areas of their profession; the second Michigan Mentorship Academy, which highlights our department’s mentorship programs, along with tips on how to be both a great mentee and mentor; and finally, we hosted our second cohort of the Coaching Academy, a program that helps extend coaching competencies to support professional and leadership development, with fourteen faculty and staff participating in this seven-month development program.
Innovation
The Mini-Sabbatical Program was reinstated this past year after a pandemic pause. This program is an opportunity for faculty to spend dedicated time toward developing their clinical, academic, or educational interests over an eight-week period. During this time, faculty are excused from clinical and administrative duties in order to provide time for immersion and deepening one’s knowledge and interests in the topic of their choice. This year, we will have six faculty members from different sections of surgery go on their sabbaticals around the world. The Center for Surgical Innovation (CSI) mentored its fourth annual cohort of Michigan Surgical Innovation Accelerator funded projects. The CSI also launched a new resident-focused Surgical Innovation Discovery Course which was designed to enhance idea exploration and prototype development for clinical-based problems.
Outreach
The Center for Global Surgery hosted its annual symposium, highlighting relevant research and clinical work within our department and other departments at U-M. The Doctors of Tomorrow (DoT) Program celebrates their 11th year serving 9-12th grade students at Cass Technical High School and now The School at Marygrove through longitudinal mentorship with M1 students; The Doctors of Tomorrow (DoT) proudly hosted their 5th Annual Diversity in Medicine conference, entitled “The Past, Present, and Future.” The Department of Surgery hosted the 2023 HOPE Symposium, welcoming keynote speaker Dr. Marc Nivet and many educational champions to collaborate on strengthening pathways in the medical ecosystem. As a project team lead, we contributed to a successful second annual Youth Summit at the Big House. The Department of Surgery provided simulations from Critical Care, the HOPE Collaborative, the ALL-SAFE Global Surgery team, and the Center for Surgical Innovation.
Research Center Highlights
Center for Basic & Translational Science
CBATS continues its mission to support the basic and translational science efforts of the Department of Surgery. Biweekly hybrid meetings have brought together researchers from across the campus to share ideas, foster collaboration and train future leaders in medical science. CBATS has hosted visiting speakers who introduced novel scientific techniques and allowed for networking with departmental scientists and trainees. Funding announcements for CBATS mini-grants have provided investment in projects that are near the funding stage to further support members. In the coming year we will expand our training to include courses in experimental design, career development, grant writing and information about the promotion process.
Center for Global Surgery
The Michigan Center for Global Surgery selected their first global surgery fellow, Dr. Brigit Baglien. The center, along with LFR International, has grown international programming for over 6,500 emergency first responders across five countries, developed a massive open online course for first responder education, investigated novel mobile phone technology for EMS dispatch in resource-limited settings and fostered partnerships with several major university and federal government partners around the world. Dr. Gifty Kwakye and colleagues, with the assistance of a multi-institutional and multi-national team, created the first colorectal surgery fellowship program in Sub-Saharan Africa outside of South Africa. Dr. Grace Kim and her team have continued work on ALL-SAFE, the portable laparoscopic training system, winning the Grand Prize of the Global Surgery Training Challenge, supported by the Intuitive Foundation, and forged connections with COSECSA and WACS to bring laparoscopy to sub-Saharan Africa.
Center for Healthcare Outcomes and Policy
We have made enormous strides in building our community in the new hybrid environment, piloting a space redesign that forms a hub of activity in the heart of our office—our Base Camp. Our leadership team has also grown with the addition of five new directors who are leading initiatives in specific areas of our center, including analytic strategy, quantitative analytics, engagement, student research and healthcare administration. We have also expanded our training opportunities to include a two-year program with didactic and experiential learning in healthcare administration. Faculty have also been awarded numerous K, R, and U-level grants as well as a successful T32 renewal in health services research and obesity-related disease. Our community continues to grow as we foster an environment and culture committed to collaboration and advancements in health services research.
Center for Surgical Innovation
The Center for Surgical Innovation mentored its fourth annual cohort of Michigan Surgical Innovation Accelerator funded projects. Projects ranged from artificial intelligence/machine learning development, medical devices and therapeutics. We launched a new Surgical Innovation Discovery Course geared toward trainees to discover and explore innovative ideas through rapid-fail prototyping and customer discovery. The CSI received funding from GME innovations, The Doctors Company Foundation and the National Science Foundation to work on extended reality simulations for bedside training procedures. The CSI has three surgical innovation fellows working on innovative projects related to mixed reality simulation and novel medical device development.
Center for Surgical Training and Research
Our members have given more than 40 presentations at research conferences, grand rounds and invited presentations nationally and internationally. Dr. Gurjit Sandhu received the Distinguished Mid-Career Educator Award through the Association for Surgical Education (ASE). Dr. Brian George received the 2023 International Medical Educator of the Year Award from the Royal College. CSTAR hosted a national seminar series in collaboration with ASE and Society for Improving Medical Professional Learning (SIMPL). CSTAR PI’s received grant funding totaling $6 million with funded projects examining topics such as entrustment in the operating room, video-based micro-teaching, psychological safety, resident competence and early-career patient outcomes and transforming surgical training using precision education.
Section & Division Highlights
Section of General Surgery
Our general surgery residency program was once again ranked #1 in the nation by Doximity. Our section had three successful faculty promotions and hired six new faculty members. We also appointed four new professorships. The section submitted 81 grant proposals and was awarded 33 extramural grants. A total of $24.6M in direct and indirect funds was awarded. We also successfully started clinical innovative programs including the radio frequency ablation thyroid program and LINX anti-reflux, and became an accredited Bariatric Center of Excellence at Chelsea.
Section of Oral & Maxillofacial Surgery/Hospital Dentistry
We were honored with the prestigious Stephen B. Milam Award for achieving the highest-scored research support grant. This accolade was bestowed upon us for our study on Estrogen Receptor Signaling in Oral Squamous Cell Carcinoma. The non-ACGME clinical Fellowship in temporomandibular joint surgery has experienced remarkable growth, and we welcomed two new fellows who will contribute their expertise and enrich our program. We are proud to report another consecutive year of achieving the highest RVUs in the history of our section. These accomplishments reflect the collective efforts and dedication of our team, and we look forward to continued growth and success in the future.
Section of Pediatric Surgery
We had a 100% match rate for all of our non-ACGME pediatric surgery fellowships with fellows starting in 2025. Dr. Newman received the 2023 Densler Award from the American Pediatric Surgical Association and was asked to serve on the external advisory board for St. Jude’s Children’s cancer center. Dr. Gadepalli became the pediatric surgery fellowship program director and his R01 was funded. Dr. Arnold led the Children’s Intestinal Rehabilitation Program and served as OR Director. Dr. Mychaliska was selected Co-President of the International Fetal Medicine and Surgery Society. Dr. Perrone became the president-elect of the Michigan Chapter of the ACS and vice chair/chair-elect of the North American Fetal Surgery Network. Dr. Speck became Director of Clinical Research, launched a weekly research conference, and became the colorectal surgery director. Dr. Thirumoorthi took on a new clinical role in endocrine surgery.
Section of Plastic Surgery
The integrated Plastic Surgery Residency program was ranked #4 in the Nation by Doximity. Our residency program has transitioned its program leadership; we are grateful to Drs. Adeyiza Momoh and Erika Sears for their years of service, and we welcome the new program directors, Drs. Paige Myers and Jessica Hsu. We published 149 peer-reviewed manuscripts over the last year and our faculty have received eight large extramural grants. Our faculty are also actively engaged in an increasing number of community and health disparity/health equity studies. Dr. Brown was awarded an NIH grant to prospectively evaluate the outcomes of outpatient surgery for removal of intercostal sensory nerves as a treatment for chronic neuropathic pain following mastectomy. Dr. Erika Sears recently began work on a newly funded VA merit award (Assessing Episode-Based Surgical Quality in VA and Community Care Settings). along with collaborators from the Ann Arbor VA, Boston VA, and Palo Alto VA.
Section of Thoracic Surgery
Highlights: We welcome several new faculty members, Dr. Chigozirim Ekeke, Dr. Zarrish Khan, and our next Section Head, Dr. David Odell, as well as colleagues Dr. Betsy Colwell at University of Michigan Health-West and Dr. James Fenton at MyMichigan Health. Dr. Rishindra Reddy has helped the Center for Surgical Innovation fellows obtain $450K in innovation grant funding in mixed reality in medical education. Dr. Reddy has also led the MSTCVS Thoracic Quality Collaborative over the past year with new initiatives to collaborate with the other oncology and surgery collaboratives to improve care for thoracic malignancies at a statewide level. We continue to develop the Robotic Bronchoscopy program with Interventional Pulmonology, and we are actively enrolling lung cancer patients in collaborative trials through the Thoracic Surgery Oncology Group including the LEADER trial sponsored by the Lung Cancer Mutation Consortium (LCMC). Our team is also in the process of activating a clinical trial funded by the NHLBI evaluating lung transplant recipient exosome phenotypes and the risk of primary graft dysfunction and acute lung allograft dysfunction in collaboration with the University of Washington and University of Wisconsin.
Section of Transplant Surgery
Last year was our busiest clinical year, and we performed 26 abdominal transplants on children and 365 on adults, including successful living donor kidney and liver programs. Our forward-thinking approach incorporates new technology and adapts to evolving regulatory requirements in transplant care. We are making a global impact through pioneering partnerships, including performing the first transplants in Rwanda. Supporting the growth of the next generation of surgeons, we have two general surgery residents matched into the field. Our faculty secures extramural research funding from diverse sources, such as NIH, Michigan DHHS, and Medicare, driving medical innovation. We lead quality improvement efforts statewide, including a $20M partnership with Medicaid to build health data infrastructure. In addition, we have implemented novel warm perfusion technologies, enabling the "all night" transplants to be delayed to 7AM to provide more flexibility for patients and providers. Our commitment to growth continues with the addition of two new faculty recruits.
Section of Vascular Surgery
We celebrated Dr. Wakefield’s retirement and his 45 years at Michigan Medicine, including his leadership to the section and the Frankel Cardiovascular Center. We also welcomed two new assistant professors, Dr. Robert Beaulieu and Dr. Frank Davis. Dr. Eliason was awarded the Coran Faculty Teaching Award and the 2023 Faculty Excellence in Education award. Our faculty had a total of 107 publications this year, and we have seen sharp growth in NIH award dollars, increasing total award dollars by 49.5% since 2020. New awards in 2023 included an R35, an F31, two F32s, and a T32, which totaled over $4 million. Dr. Katherine Gallagher received an R35 Outstanding Investigator Award, securing $7.3 million in research support for “The epigenetic regulation of inflammation in tissue repair and vascular disease.” Dr. Vemuri and Dr. Henke started participating in a multi-disciplinary Dialysis Access Clinic with the transplant surgery team and opened a general vascular surgery clinic at St. Joe’s Hospital in Chelsea, MI.
Division of Anatomical Sciences
Our faculty taught more than 1,300 students this year, with increased enrollment in ANAT 303 and our Massive Open Online Course (MOOC) anatomy series on Coursera, EdX, and FutureLearn. We continued consistent leadership in open-access anatomy learning resources through the BlueLink project, which is used worldwide at over 150 institutions. It has led to an increase in development of open-access, three-dimensional scans and modules, and promotes access and equity in educational resources for anatomy learners worldwide.
Our Team Highlights
New Faculty Members
- Joseph Church, MD: Pediatric Surgery
- Chigozirim Ekeke, MD: Thoracic Surgery
- Ben Ferguson, MD, PhD: Hepatopancreatobiliary Surgery
- Danielle Haakinson, MD: Transplant Surgery
- Molly Hunter, MD: Acute Care Surgery
- Hope T. Jackson, MD: Minimally Invasive Surgery
- Zarrish Khan, MD: Thoracic Surgery
- Lauren Krumeich, MD, MS: Endocrine Surgery
- Peng Liao, PhD: Department of Surgery
- Lauren Marquette, MD: Plastic Surgery
- Lavika Mor, BDS: Oral & Maxillofacial Surgery
- David Odell, MD, MS: Thoracic Surgery
- Robin Petroze, MD, MPH: Pediatric Surgery
- Noah Saad, MD: Plastic Surgery
- Jenny Shao, MD: Minimally Invasive Surgery
- Kyle Sheetz, MD, MS: Transplant Surgery
- Hunter Underwood, MD: Endocrine Surgery
- Jiali Yu, PhD: Department of Surgery
- Jiajia Zhou, PhD: Department of Surgery
Faculty Promotions & Professorships
- Dr. Kevin Chung: William C. Grabb Distinguished University Professor of Surgery
- Dr. Samir Gadepalli: Daniel H. Teitelbaum, MD Collegiate Professor
- Dr. Michael A. Holinstat: Professor of Internal Medicine and Surgery
- Dr. Cindy Hsu: Associate Professor of Emergency Medicine and Surgery
- Dr. Tasha Hughes: Clinical Associate Professor of Surgery
- Dr. Andrew Ibrahim: Maud T. Lane Research Professor
- Dr. Gifty Kwakye: Arthur W. Fleming, M.D. Research Professor
- Dr. Suresh Madathilparambil: Associate Research Scientist of Surgery
- Dr. Justine Moe: Clinical Associate Professor of Surgery
- Dr. Daniel Myers: Conrad & Caroline Jobst Research Professor in Vascular Surgery
- Dr. Nicholas Osborne: Ramon Berguer, M.D., Ph.D. Research Professor of Vascular Surgery
- Dr. Dana Telem: Professor of Surgery with Tenure
- Dr. Chandu Vemuri: Marion and David Handleman Research Professor of Vascular Surgery
- Dr. Christian J. Vercler: Clinical Professor of Neurosurgery and Surgery
- Dr. Seth A. Waits: Clinical Associate Professor of Surgery
- Dr. Jennifer Waljee: Professor of Surgery with Tenure and Professor of Orthopaedic Surgery
New Residents
- Sonali Biswas, MD: Integrated Plastic Surgery Residency
- Amanda Bogue, DDS: Hospital Dentistry General Practice Residency
- Devon Cassidy, MD: General Surgery Residency
- Sagar Chadha, DDS: Oral & Maxillofacial Surgery Residency
- Monica Chavan, MD: General Surgery Residency (Preliminary - Interventional Radiology)
- Katherine Coburn, MD, PhD: General Surgery Residency
- Dillon Dejam, MD: Integrated Plastic Surgery Residency
- John Domini, MD: General Surgery Residency (Preliminary - Interventional Radiology)
- Thomas DeLay, MD: Integrated Thoracic Surgery Residency
- Grace Garry, DDS: Hospital Dentistry General Practice Residency
- Daniela Gomez Zubieta, MD: General Surgery Residency (Preliminary)
- Timothy Gilbert, MD: General Surgery Residency (Preliminary)
- Emily Graham, MD: Integrated Plastic Surgery Residency
- Lauren Hensick, MS, DMD: Orofacial Pain Residency
- Theodore Hu, MD: General Surgery Residency
- Yousef Ibrahim, MD: General Surgery Residency
- Lindsay Janes, MD: General Surgery Residency
- Manpreet Kaur, DDS: Hospital Dentistry General Practice Residency
- Abed Kawakibi, MD: General Surgery Residency (Preliminary)
- Adhithi Kesari, DMD: Oral & Maxillofacial Surgery Residency
- Trever Koester, MD: General Surgery Residency
- Timothy Kravchenko, MD: General Surgery Residency
- Jennifer Lee, MD, MS: Integrated Plastic Surgery Residency
- Andrew Navarro, MD: General Surgery Residency (Preliminary - Interventional Radiology)
- Sonali Reddy, MD: Integrated Vascular Surgery Residency
- Morgan Ritchie, DDS: Hospital Dentistry General Practice Residency
- Rebecca Shembarger, DDS: Oral & Maxillofacial Surgery Residency
- Mami Sow, MD: Integrated Thoracic Surgery Residency
- Haley Talbot-Stetsko, MD: General Surgery Residency (Preliminary)
- Victoria Waynick, DDS: Hospital Dentistry General Practice Residency
Culture Crew
The Culture Crew, convened by the Vice Chair for Faculty Development, is charged with leading efforts for intentional culture design in the Department of Surgery. We strive to foster an environment of excellence where everyone can succeed and take pride in our work, mental and physical health are priorities, and differences and diversity are valued and respected. When individuals come to work whole and well, we can accomplish the extraordinary together.
Task teams have focused on programs such as #WallsDoTalk, Cultural Complications, COMPASS Training, Michigan Action Progress System (MAPS), and workforce diversity outreach through the HOPE Collaborative, Doctors of Tomorrow, and the Michigan Medicine Youth Summit at the Big House.
2023 Culture Crew Retreat and Department Well-Being
The Culture Crew hosted the annual Spring Retreat for faculty, staff, and APPs across sections, with dedicated time to gather to discuss departmental priorities and action plans to meet the needs of our teams. The theme of the 2023 Culture Crew Retreat was “Giving Grace: Mental Health and Culture Design in a Changed World.” Work groups candidly addressed wellness, burnout, and retention issues, analyzed 2022 engagement data, and established a strategic focus on well-being and supporting teams to enhance culture at the section level.



