Program History
The University of Michigan kidney and pancreas transplant program recently reached an important milestone — it's 7,000th kidney transplant since U-M surgeons conducted the first back in 1964. It's a notable achievement for the program and, most importantly, for patients. New clinical approaches, research discoveries, outreach efforts and changes to national organ allocation policies have made kidney transplant, and live donation, an option for a greater number of people.
The procedure has evolved a great deal since that first transplant — a living donation from one 15-year-old identical twin to her sister, performed by Professor of Surgery Emeritus, Dr. Jeremiah G. Turcotte. (The two did well and even returned to U-M in 2014 to celebrate the Transplant Center's 50th anniversary.) At the time, the procedure was only about a decade old and largely limited to live, twin donors, which eliminated the risk of rejection and the need for immunosuppression medications.
Today, national kidney transplant outcomes carry a one-year patient survival rate of about 96% to 97% and an organ survival rate, also known as graft survival, of between about 93% and 98%. And while those outcomes — and having completed more than 7,000 transplants — might suggest that kidney transplant at U-M has become routine, it is anything but. That's in part because U-M accepts complex and riskier cases often turned down by other transplant centers.
Drawing on Resources
"While sometimes people think of the transplant surgeons and transplant nephrologists as the cornerstones of any kidney transplant program, at U-M we take an aggressively multidiscliplinary approach. We have so many well-developed teams in other specialties that let us transplant patients other centers won't," said Dr. Kenneth Woodside, associate professor and transplant surgeon. "We have one of the world's best intensive-care units if there are complications; we have similarly strong programs in cardiology and anesthesiology as well as transplant infectious disease and transplant psychiatry — all important services to caring for the kidney and the patient." This multidisciplinary expertise allows UM to take on many patients that are higher risk.
The program also has an active outreach group that, among other activities, visits dialysis units and puts on programs around the state to educate patients about transplant and living donation.
While dialysis can offer hope to some patients, particularly those who are not candidates for transplant, it doesn't replace normal, continuous kidney function in terms of the volume of fluid removal and toxin filtration. That translates to greatly improved life expectancy. Kidney transplant is also less expensive than dialysis.
Yet, getting patients on the U-M Transplant Center's wait list through the United Network for Organ Sharing remains a challenge. Being turned down by other centers can lead patients to believe it's not an option for them. Others have fears or concerns and don't investigate further. Still others don't realize how it could potentially improve their life span or quality of life.
Improving Access
Education and getting listed are key steps but, with need far exceeding supply of deceased donor kidneys, the time to transplant — often several years — can be too long for a patient with end-stage disease. Between 200 and 250 patients per year receive kidney transplants at Michigan Medicine.
Live donation significantly shortens the process, and these procedures comprise about 40% of the kidney transplants performed at U-M. When patients can't find a living donor on their own, or the donor is incompatible, the program can help. In 2007, the U-M Transplant Center began offering paired kidney donation, in which a patient's (incompatible) donor can provide a kidney to another recipient on the wait list; the patient then receives a kidney from a closer match.
Crossing Borders
The program's longevity, size, and successes have enabled faculty to help expand access to kidney transplants far beyond the state. Led by Dr. Jeffrey Punch, the Jeremiah and Claire Turcotte Professor of Surgery, a U-M team of transplant surgeons, nurses and social workers has helped establish the first transplant center in Ethiopia.
Dr. Punch began working with the Ethiopian Ministry of Health in 2013. Over the ensuing years and many visits, Dr. Punch and colleagues, including Dr. Woodside, trained the first cohort of Transplant Surgery and Transplant Nephrology fellows at Saint Paul's Millennium Medical College in Addis Ababa. The four fellows graduated in late 2018 and have performed about 130 transplants to date. The impact will only widen as these surgeons soon begin training other physicians in-country.
On the Horizon
Although strictly speaking transplant is not a cure for kidney failure, since patients still need lifelong medication to prevent rejection, Dr. Woodside is optimistic as he looks ahead. "We lose a lot of kidneys to chronic disease states. That's the next challenge. We've gotten good at preventing rejection, so now we can work on minimizing the impact of chronic diseases that affect the recipient's new kidney. In a way, it's a good problem to have."
The expansion of the U-M Health System's hospital network is good news, too, bringing more patients in to be evaluated and listed, including those higher-risk patients who are safest having the procedure performed at a comprehensive, quaternary care hospital. "We always say how medicine is a team sport," Dr. Woodside said, "and I think transplant might be the field that demonstrates that the best."
Quick Facts:
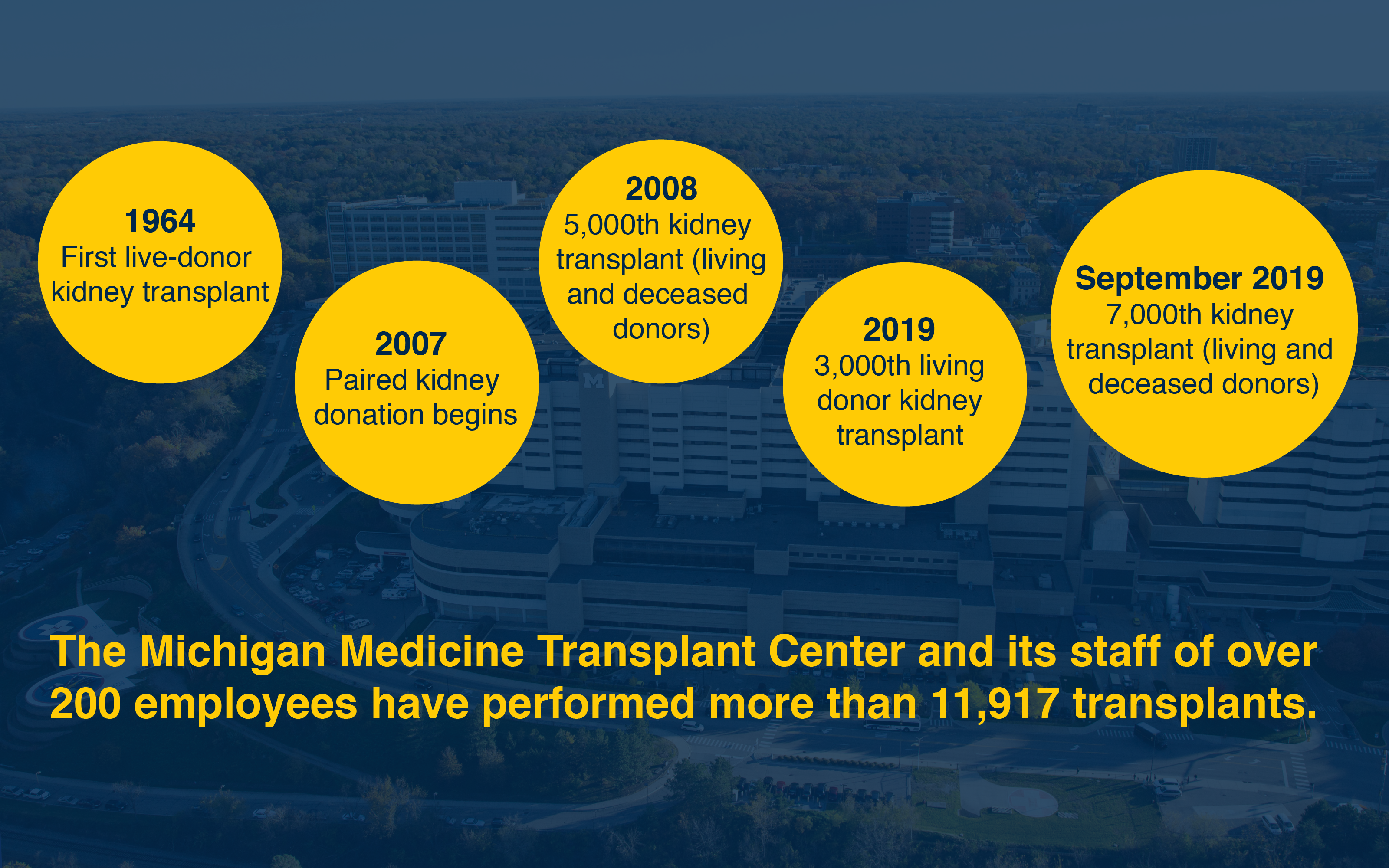
- 1964: First live-donor kidney transplant
- 2007: Paired kidney donation begins
- 2008: 5,000th kidney transplant (living and deceased donors)
- 2019: 3,000th living donor kidney transplant
- September 2019: 7,000th kidney transplant (living and deceased donors)
Article by Kim Roth
