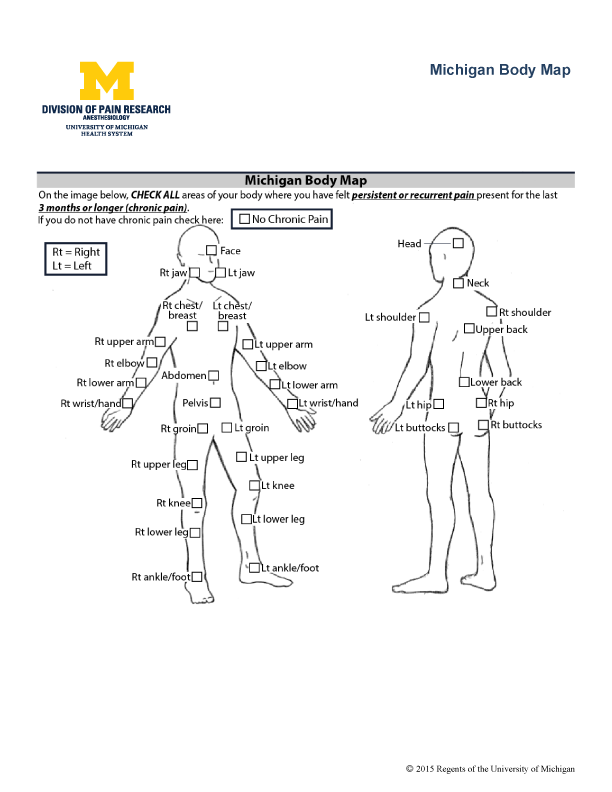
- Body maps have been used for many decades to assess the location of pain complaints
- The Michigan Body Map (MBM) is a self-report measure to assess body areas of chronic pain
- The MBM can also quantify the degree of widespread body pain when assessing for centralized pain features (e.g. fibromyalgia like presentation
- MBM demonstrates utility, reliability, and construct validity
- MBM can be used to accurately assess distribution and spread of body pain
- MBM is an efficient and accurate element of the fibromyalgia survey score
For your use, these measures, along with scoring and SPSS syntax, are available for downloading:
- Michigan Body Map, current version
- Michigan Body Map, original version
- Scoring and SPSS Syntax for both versions of MBM- 2 tabs/pages in the Excel document
- Michigan Body Map, Spanish version
Chad Brummett, MD provides an overview of the self-reporting measure in a newly released video based on an article in Pain
We developed the Michigan Body Map (MBM) as a self-report measure to assess body areas where chronic pain is experienced and to specifically quantify the degree of widespread body pain when assessing for centralized pain features (e.g., fibromyalgia-like presentation). A total of 402 patients completed the measure in five distinct studies to support the validation of the original and a revised version of the MBM.
Administration is rapid 39-44 sec and errors for the original MBM were detected in only 7.2% of the possible body areas. Most errors underestimated the number of painful areas or represented confusion in determining the right versus left side. The MBM was preferred (p=0.013) and felt to better depict pain location (p=0.001) when compared to the Widespread Pain Index checklist of the 2011 Fibromyalgia Survey Criteria, but participants did not express any preference between the MBM and Brief Pain Inventory body map.
Based on the data from the first three studies, a revised version of the MBM was created including a front and back body image and improved guidance on right-sidedness versus left. The revised MBM was preferred when compared to the original and more accurate in depicting painful body areas (p=0.004). Furthermore, the revised MBM showed convergent and discriminant validity with other self-report measures of pain, mood and function.
In conclusion, the MBM demonstrated utility, reliability and construct validity. This new measure can be used to accurately assess for the distribution or widespreadedness of bodily pain as an element of the fibromyalgia survey score.