About Us:
Our lab group investigates ways to explore the optimal use of images and the signals from which they are conventionally reconstructed to optimally support precision radiation therapy. Our projects include investigations related to:
- Advancing precise Image-Guided Radiotherapy (IGRT)
- Developing and improving dynamic human models
- Studying the complexity of therapeutic decisions and the sparsity of information sufficient to justify decisions throughout the radiotherapy process
- MRI-guided radiotherapy
- Projection-to-volume modeling of pose, configuration, and movement
Projects
MRI-Only Treatment Planning and Image Guidance
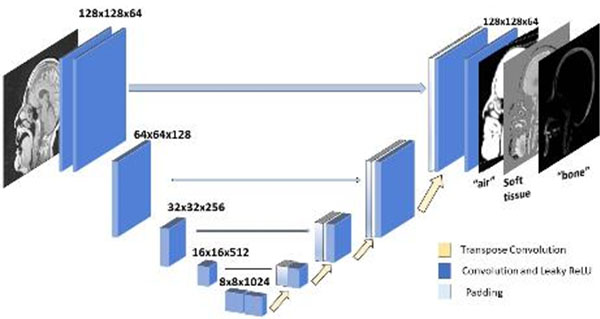
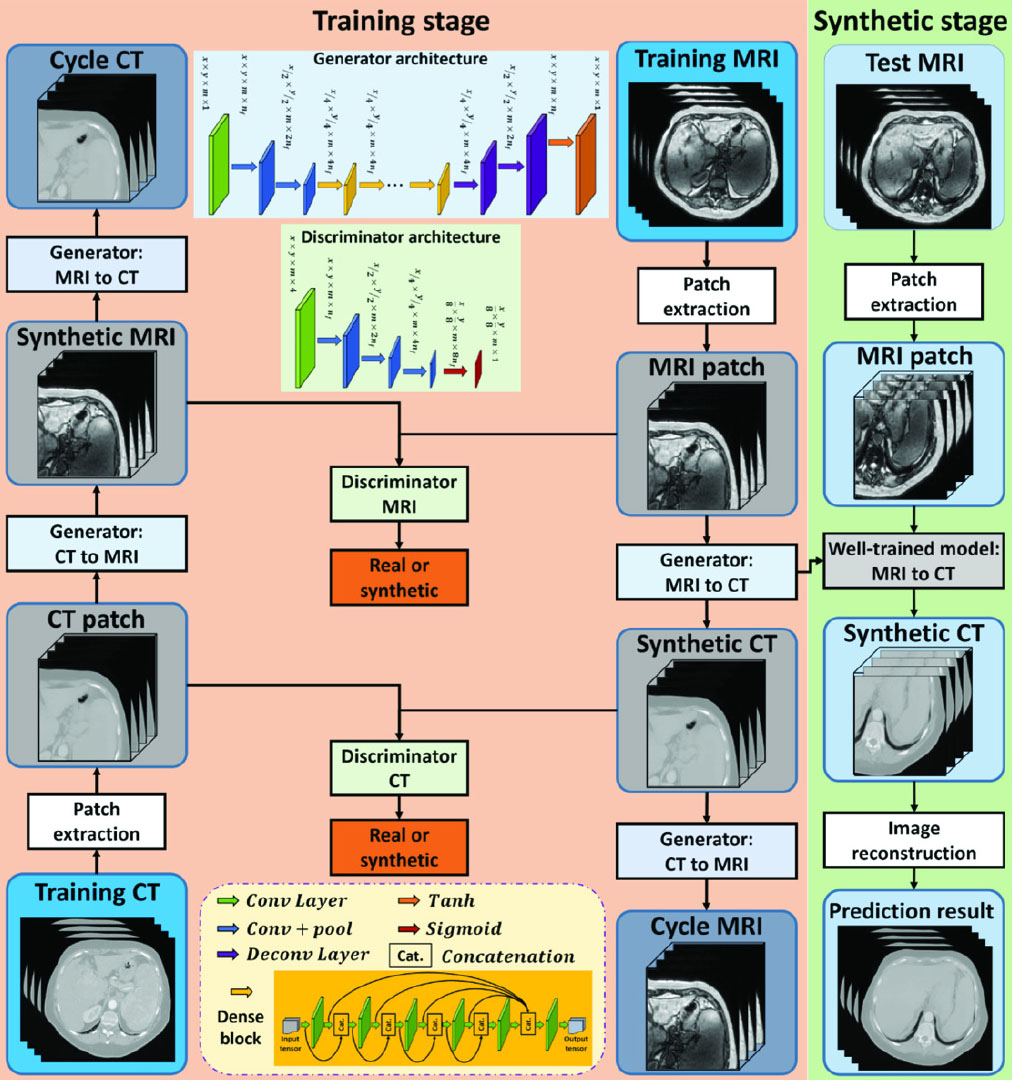
Our lab investigates the development of patient models that support both the planning of radiation therapy as well as image-guided patient positioning. Patient models are derived from a combination of the intensity patterns of different tissues across different MRI contrasts, as well as through the integration of prior knowledge of anatomic shapes (e.g. pelvic bones) within a population of patients. Synthetic CT models of the head have been developed and clinical implementation is expanding from initial support of whole-brain radiotherapy to more focal treatments of glioblastomas and stereotactic treatments of multiple metastases.
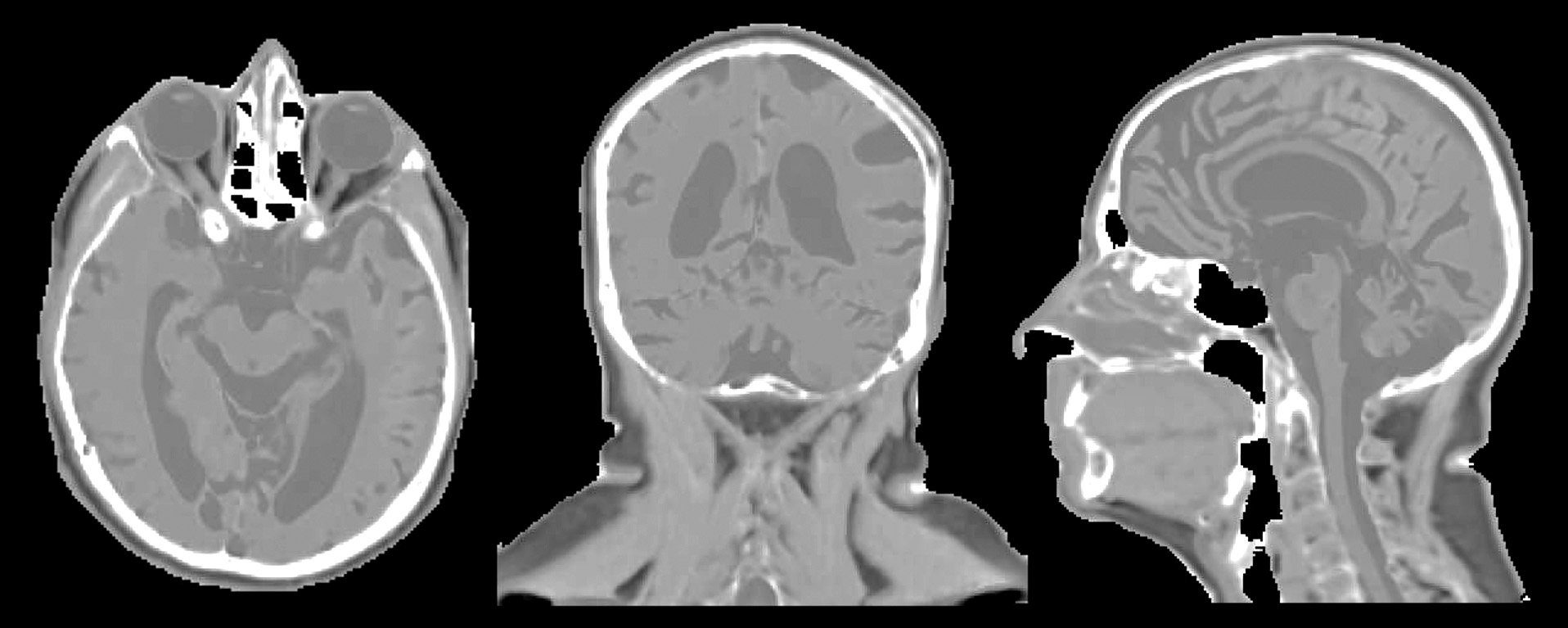
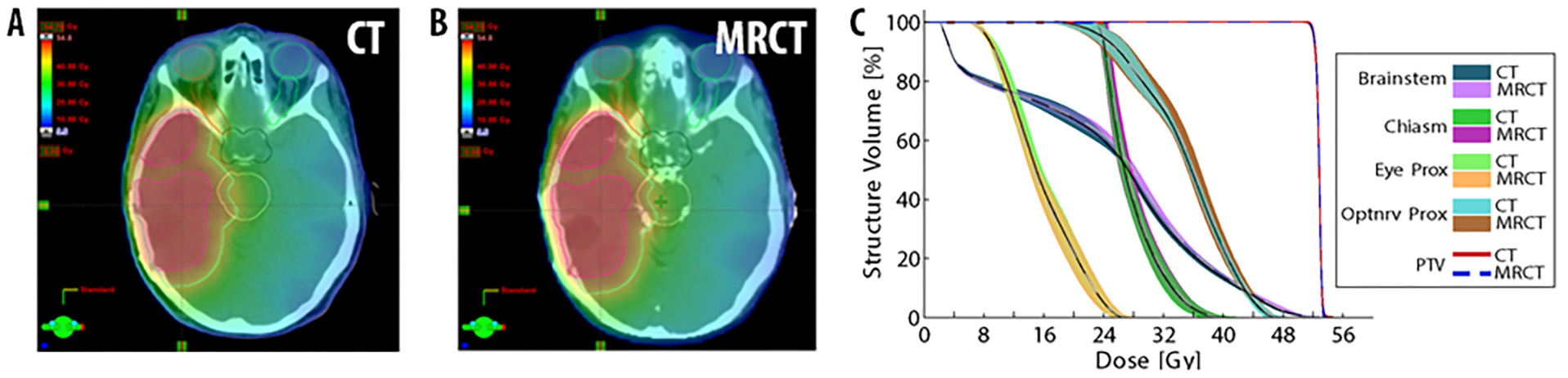
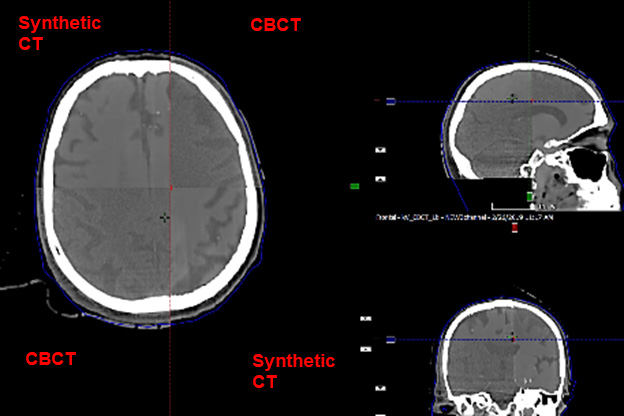
In the pelvis, statistical shape models have been used to improve the accuracy and reduce the scanning complexity of synthetic CT modeling. Principal Component Analysis of a statistical bone shape model extracted from deformable modeling of pelvic volumes across a population of previous patients yields a simple description of a bone mask that separates bone from air in the pelvis. This methodology has been demonstrated to provide sufficient accuracy for IMRT planning in the female pelvis, and is currently being translated to a robust software tool for clinical implementation.
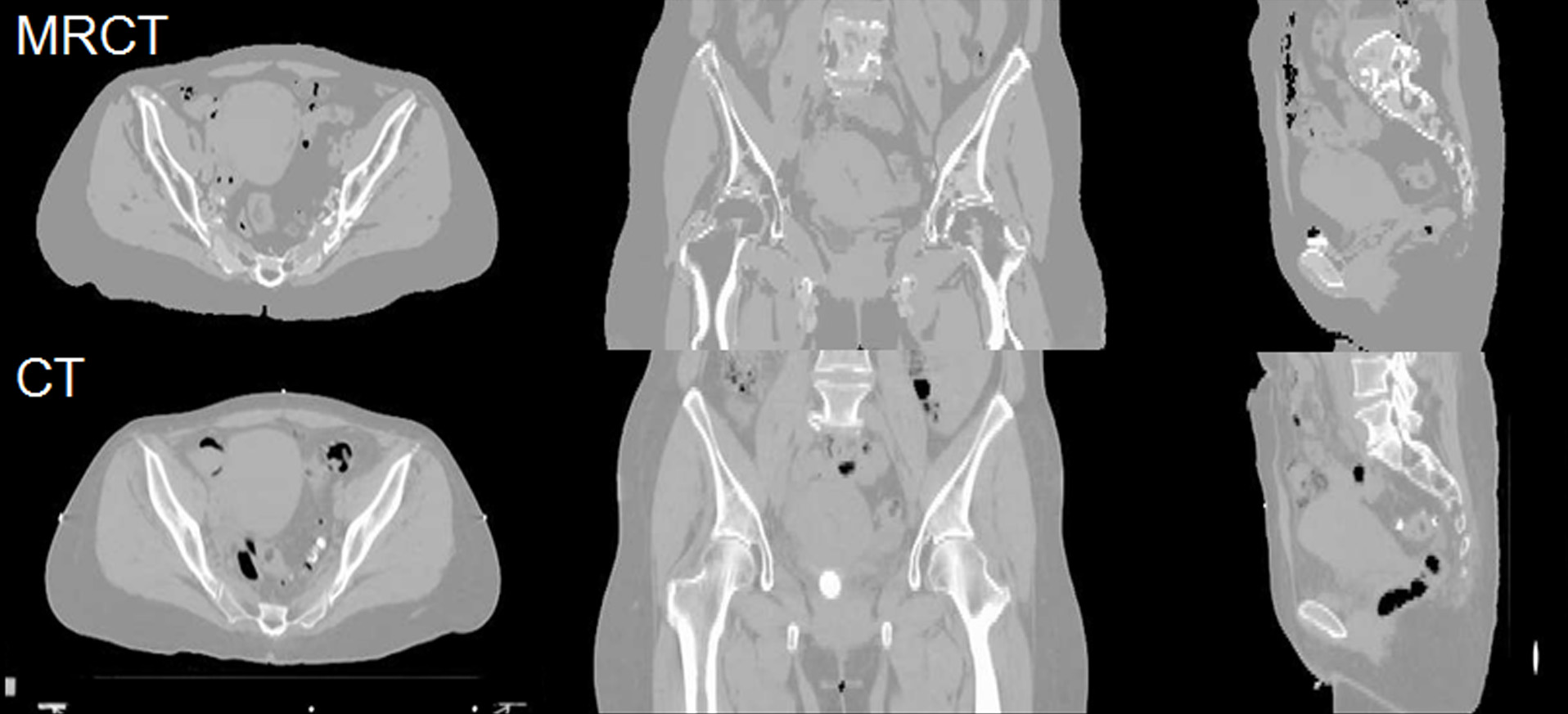
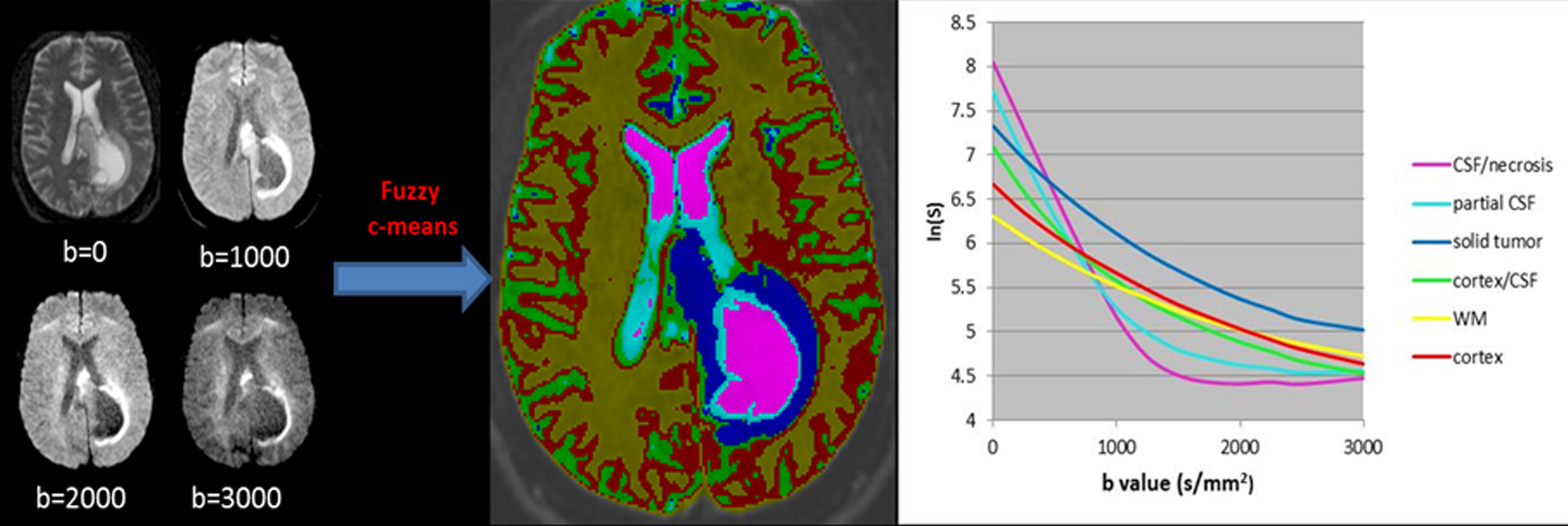
Biological Sparsity
MR imaging is typically slow and subject to artifacts from several factors that limit its utility for supporting a number of radiation therapy tasks, including target definition and understanding and reacting to motion. Fortunately, sufficient sparsity exists to potentially support these tasks with more efficient sampling and/or intelligent reconstruction techniques. Our lab is currently investigating sparsity of biological mapping of diffusion, morphological mapping of anatomic structure, and mapping hierarchical motion states of patients.
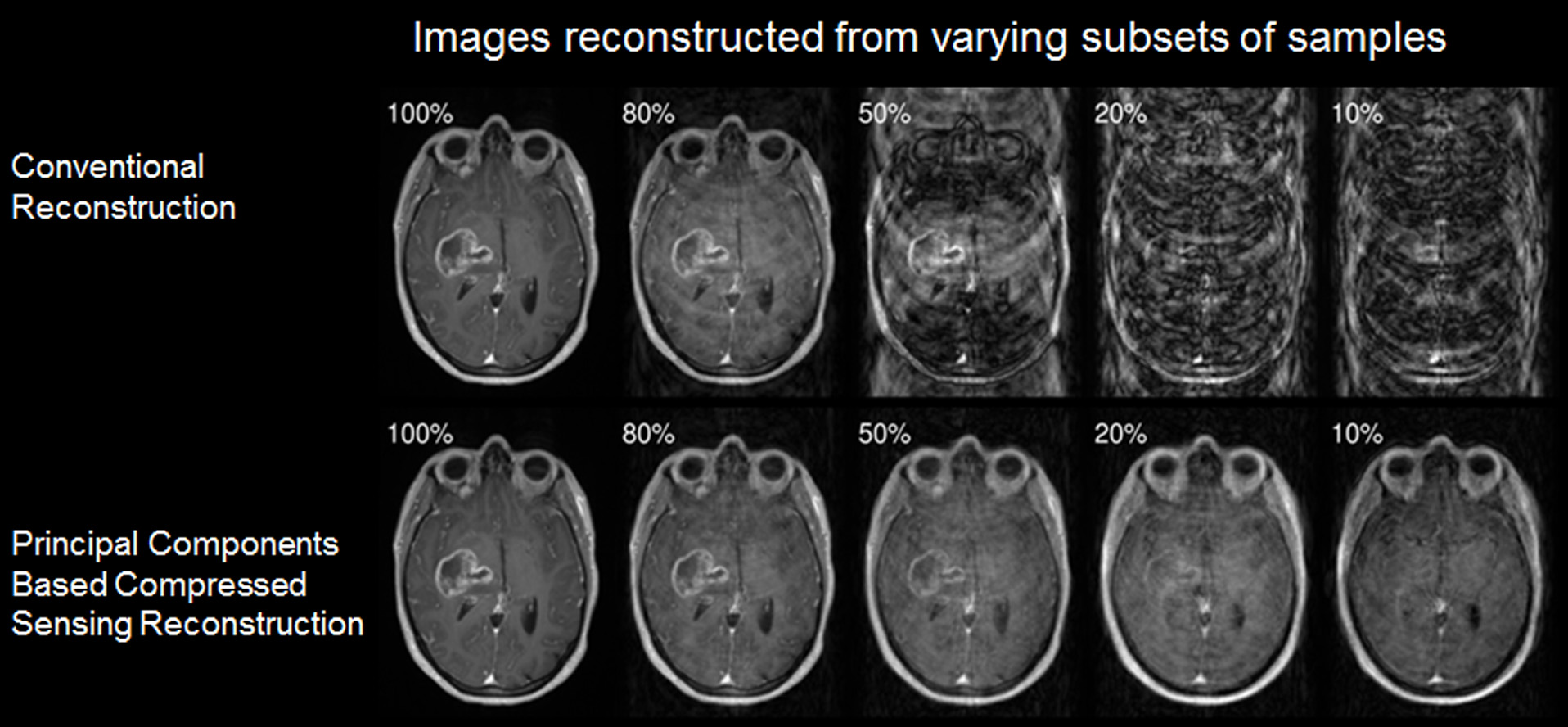
Morphological Sparsity
MR imaging is typically slow and subject to artifacts from several factors that limit its utility for supporting a number of radiation therapy tasks, including target definition and understanding and reacting to motion. Fortunately, sufficient sparsity exists to potentially support these tasks with more efficient sampling and/or intelligent reconstruction techniques. Our lab is currently investigating sparsity of biological mapping of diffusion, morphological mapping of anatomic structure, and mapping hierarchical motion states of patients.
Hierarchical Motion of the Abdomen from Dynamic MR Signals
MR imaging is typically slow and subject to artifacts from several factors that limit its utility for supporting a number of radiation therapy tasks, including target definition and understanding and reacting to motion. Fortunately, sufficient sparsity exists to potentially support these tasks with more efficient sampling and/or intelligent reconstruction techniques. Our lab is currently investigating sparsity of biological mapping of diffusion, morphological mapping of anatomic structure, and mapping hierarchical motion states of patients.
Join Us:
If you are interested in joining us, please email James Balter, PhD.
Laboratory Lead




