
The Child and Adolescent Psychiatry Fellowship at Michigan Medicine has long been recognized as one of the nation’s foremost programs for training leaders in the field. Its rigorous yet flexible course of training produces clinicians with outstanding skills in diagnostic assessment, empirically-based psychotherapies, somatic treatment, and consultation. The section also enthusiastically supports residents interested in academic careers, research, and medical education, through faculty actively engaged in diverse research and scholarly activities. Child psychiatry residents may enroll in a research training track that merges research and clinical training.
Who Should Consider Training in Child/Adolescent Psychiatry?
Child psychiatry training is valuable not only for physicians who have decided upon a career working with children, but also for psychiatrists who demand a fuller appreciation of behavior and psychopathology from longitudinal and developmental perspectives. Many important psychiatric disorders, including behavior disorders and pervasive developmental disorders, begin in childhood. Other disorders commonly viewed as the domain of adult psychiatry, including schizophrenia and bipolar disorder, typically crystallize in adolescence or early adulthood, with early signs sometimes evident in infancy. Psychosocial adversity in early life reverberates through the lifespan and most theories of personality development emphasize early developmental influences and predispositions.
For these reasons, child psychiatrists offer unique perspectives on psychopathology across the life cycle. Furthermore, as psychiatry seeks a niche as a primary care specialty, the capacity to treat whole families spanning several generations of psychopathology will become increasingly valuable.
In practice, many adult psychiatrists treat adolescents. Those with certificates of training or board certification in child/adolescent psychiatry have a wider range of employment options. Salaried child psychiatrists frequently earn a premium. Child psychiatry is consistently among the most sought after specialties in medicine.
Program Overview
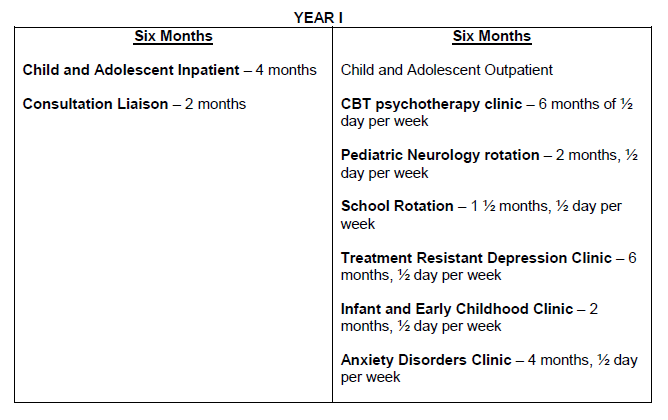
The Child and Adolescent Psychiatry fellowship program at The University of Michigan is a fully accredited two-year program that accepts six fellows each year. During the two years of training, child psychiatry fellows spend six months covering the inpatient unit and consultation services and 18 months in our outpatient clinics located at the Depression Center and Ambulatory Psychiatry facility, in the Rachel Upjohn Building. This center, which opened in October 2006, is the first among the National Network of Depression Centers and combines clinical expertise, cutting edge research, and innovative teaching for a new generation of leaders in child and adolescent psychiatry. Throughout the rotations, child psychiatry fellows are provided with protected time to attend the core lecture series, journal clubs and collaborative case conferences.
"I feel very fortunate to attend the Child and Adolescent Psychiatry fellowship program at University of Michigan. The program emphasizes education and training value above productivity. It also promotes resident wellness and work-life balance. There is an amazing amount of faculty/staff support, particularly from our program director and administrative specialists. Between exposure to numerous sub-specialty clinics and the ability to individualize my training based on my clinical interests, I feel more than ready to practice child psychiatry in any setting after graduation."
~ Katie McCormick-Deaton, D.O., 2nd year fellow
"This program offers a wide variety of unique experiences that you can't get anywhere else. I was especially impressed with the new inpatient child psychiatry unit. I learned so much about child and adolescent psychopathology including using ECT for treatment resistant depression and adolescent onset psychosis. You can't get that experience anywhere else. If I had to choose all over again I would choose University of Michigan"
~ Rachel Bokelman, M.D., 2nd year fellow
Rotations and Clinical Activity
Inpatient and Consultation Liaison Service
The Child and Adolescent Psychiatry inpatient unit is a 16 bed unit located at Mott Children’s Hospital, part of the University of Michigan Health System. There are typically three first year child and adolescent psychiatry fellows (CF-1’s) on service at any given time along with rotating adult psychiatry residents and medical students. Under the supervision of two faculty members, child psychiatry fellows provide comprehensive and highly specialized treatments to children and adolescents with complex and severe mental health challenges. As a part of the multi-disciplinary team, fellows work in a supportive and nurturing environment while learning the interface between child psychiatry, consultation-liaison service, social work, nursing, education, occupational recreational therapy and nutritionist services. Fellows also have the unique experience of evaluating and treating severe depression with ECT, which is rare in other institutions.
For two months of this rotation, one fellow is dedicated to the consultation service, which provides clinical and educational services at Mott Children’s Hospital. Consultations are provided to all pediatrics inpatient services, including general pediatric inpatient services, pediatric intensive care, neonatal intensive care unit, pediatric physical medicine and rehabilitation, pediatric neurology, and other pediatric subspecialty services.
Outpatient Rotations
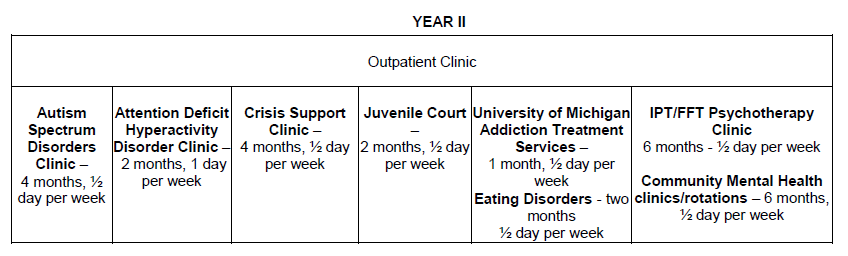
During outpatient rotations, a full-time clinical commitment consists of approximately 24 hours of direct patient contact per week. Child psychiatry outpatient services includes both general and specialty clinics. Child psychiatry fellows rotate through these clinics throughout their 18 months.
CBT and IPT/FFT Clinics: One half-day per week for six months per clinic. Fellows receive didactics and training in both cognitive behavioral therapy and interpersonal therapy/family focused therapy. Supervisors for these clinics include expert social work and psychology faculty members. Each fellow is expected to carry two therapy cases. Fellows receive real-time supervision and feedback via a one-way mirror.
School Rotation: One-half day per week for two months. During the first year of training, fellows spend time in the school setting (elementary and high schools). This rotation allows fellows to observe normal childhood development. Child psychiatrists often need to distinguish between normal variance in development and psychiatric illness.
ADHD Clinic: One day per week for two months. Fellows participate in clinical interviews, observe neuropsychological testing, and collaborate with neuropsychology to determine diagnosis and treatment plans. This clinic provides fellows with the opportunity to take an in-depth look at ADHD and potential co-morbidities.
ASD Clinic: One half-day per week for four months. This multidisciplinary clinic consists of psychiatrists, speech and language pathologists, neuropsychologists and social workers. The team works together to evaluate children with suspected autistic spectrum disorders, clarify diagnoses and develop treatment plans. This is a unique educational experience that trains fellows to recognize and treat this disorder.
Anxiety Disorders Clinic: One half-day per week for four months. This clinic takes place during the first year of training. This clinic allows for training in the diagnosis and management of anxiety disorders, including OCD, GAD, social phobia, and tic disorders. Fellows are supervised by leading experts in this field who are actively engaged in research in these areas.
Treatment Resistant Depression Clinic: One half-day per week for six months. In this clinic, fellows learn to thoroughly evaluate and manage patients with severe depression. These patients have often failed numerous medication trials prior to seeking out consultative care, with the majority of patients actively receiving ECT. Fellows also work closely with the ECT team.
Infant and Early Childhood Clinic (IECC): One half-day per week for two months. This clinic aims to serve families with identified or suspected parent-child relationship risks. The team provides early relational assessments, family/dyadic interventions, educational feedback, and referrals for intensive treatment. Fellows have the rare opportunity to work with developmental experts, with use of one-way mirror to observe behavioral assessments including The Strange Situation task, ADOS, dollhouse and story techniques, and parental scaffolding.
Community Mental Health Centers (Corner Clinic, Ypsilanti Pediatrics and Huron Valley Child Guidance Clinic): One half-day per week for six months. This rotation provides fellows the opportunity to participate in an integrated care clinic and work with low-income families. Patients have a variety of disorders, including depression, anxiety and PTSD. Fellows collaborate with medical students, adult psychiatry residents, primary care providers and case managers.
Washtenaw County Trial Court, Juvenile Division (JCWC): One half-day per week for two months. Fellows visit the Washtenaw Juvenile Court and detention center in the second year of training. The rotation is designed to augment the core lectures on forensic/legal topics provided by staff from the forensic center. During this rotation, fellows observe the juvenile court proceedings, attend assessments of court involved youth and accompany a case worker in the Intensive Probation Program on community visits.
University of Michigan Addiction Treatment Services (UMATS): One half-day per week for one month. The University of Michigan Addiction Treatment Services provide a broad continuum of diagnostic and treatment substance use services for patients thirteen years and older. Learning objectives for the UMATS rotation are met through a variety of activities, including didactics and attendance of Intensive Outpatient Program groups.
Pediatric Neurology: One half-day per week for two months. Fellows participate in an observational learning opportunity, working with attending pediatric neurologists. This clinic is a favorite of the fellows and the exposure is an important tool in studying for board exams.
Psychiatry Emergency Services (PES): Fellows take a 6-10 p.m. call shift approximately 1-2 times per month in the psychiatry emergency room, which is separate department from the medical ER. It is fully staffed with administrative personnel, social workers, psychologists, nurses and psychiatrists. PES has a collaborative and congenial atmosphere. Fellows provide emergency consultation to children, adolescents and their families.
Trainee Wellness
We continue to have a multi-layered approach to the way in which wellbeing is addressed within our curriculum. First and most important, wellbeing of our fellows is a core component of the program. As child psychiatrists, we believe that we have to take care of ourselves in order to take care of others. As a smaller program with 12 fellows, we are personally invested in the wellbeing of each trainee and work to provide them guidance, mentorship, and support throughout their training.
In terms of allowing for ability to take care of one's own physical/emotional/mental wellbeing, the University of Michigan offers a House Officer Mental Health program https://medicine.umich.edu/dept/psychiatry/programs/house-officer-mental-health-program-homhp. Also, we allow for flexibility in scheduling to allow for fellows to attend medical and psychiatric appointments.
We also give protected time for administrative tasks which as part of fellow day-to-day clinical care and do not schedule evening outpatient clinic hours to allow for fellows to have consistent work hours to help with work/life balance.
In terms of building a culture of belonging and social support, we plan field trips and a resident retreat yearly in which fellows have a chance to visit local programming related to meeting the needs of children with mental health in the community.
For additional resources available to house officers through Michigan Medicine, including an online and confidential self-screening tool, please go to the house officers section of the Wellness Office website:https://wellnessoffice.med.umich.edu/resources/for-house-officershttps://wellnessoffice.med.umich.edu/resources/for-house-officers.
For additional national resources, please go to: https://dl.acgme.org/pages/well-being-tools-resources
Advantages of Our Program
The child and adolescent psychiatry program has several advantages that distinguish it from most other leading programs. To mention a few:
- Evaluations and treatment in settings that follow diverse models of training and care, including multidisciplinary assessment, numerous sub-specialty clinics, collaborative care models, and directly monitored psychotherapy training
- Protected didactic time including
- Weekly lectures given by specialists in the field
- Research seminar focused on statistics and critical review of pivotal articles in the history of child psychiatry
- Writing workshop targeting development of scholarly work
- Journal club exploring clinical interests of each fellow
- Growth and development seminar
- Dedicated supervision time
- Faculty available to staff clinics in real-time (i.e., 1-2 faculty members are assigned to only cover supervision and do not see their own patients during that time period)
- One hour per week with a faculty member matched for clinical and research interests
- One hour per month with our program director during Resident Lunch to discuss issues and recommendations for improvement. Fellows also meet with Dr. Mohiuddin regularly during didactics and are given her personal contact information for additional concerns
- Modularized program for training in major psychotherapeutic modalities for the full spectrum of child/adolescent psychiatric referrals, including:
- Cognitive Behavioral Therapy
- Interpersonal Therapy
- Family Focused Therapy
- Motivational Interviewing
- Fellows also have the option of pursuing additional training in Dialectical Behavioral Therapy and Psychodynamic Psychotherapy
- Ten hours per week of administrative time to collaborate with therapists or specialists, communicate with schools, and complete documentation
- Outpatient clinics run from 8am-5pm, with no evening or weekend clinic requirements. The majority of clinics are located at the same site, with little travel needed during training
- One month of elective time in the second year of training, typically spread out as a half-day clinic per week. In the past, fellows have completed electives in our Eating Disorders PHP, dialectical behavioral therapy, developmental pediatrics, sleep clinic, FAS and genetics clinics, spiritual care, ECT, and pediatric collaborative care. Fellows have also dedicated their elective time towards pursuit of research or completion of international rotations
- Emphasis on scholarly and quality improvement projects, many of which have been published or presented at conferences
- Encouragement of conference attendance, with 5 days given for conferences (in addition to 20 vacation days per year) as well as $2,000 compensation for conference expenses. Additional funding is available for fellows who are presenting
- 100% board pass rate for those who took the exam in the last 5 years
- Limited call
- No 24-hour call coverage
- 4-6 Saturday half-day shifts total on the inpatient unit in the first year, none in the second year
- 1-2 calls per month from 6-10 pm in Psychiatric Emergency Services on Mondays, Tuesdays, or Wednesdays only
"I really appreciate the amount of support and supervision that our program gives to the fellows...the faculty are all incredibly knowledgeable and enthusiastic, which makes for a nice work environment"
~ Christina LaRosa, M.D., 2nd year fellow
"This is the perfect balance between clinical work and scholarly activities"
~ Nauman Khan, M.D., 1st year fellow
"One of the things I most appreciate about this program is the emphasis on education and mentorship. We have dedicated time and mentorship in learning how to read the literature in general, as well as making sure we read and understand the most critical points in the seminal articles in child psychiatry. Having someone walk you through the benchmark studies is particularly helpful to building your own clinical knowledge, as well as developing the confidence to read articles critically on your own. There is also dedicated time and mentorship in developing your own niche area of interest and research/educational activities, which I have found invaluable in planning for early career goals"
~ Laura Andersen, M.D., 2nd year fellow
How to Apply
Our Fellowship Program requires that trainees have completed a year of internship and two years in an ACGME accredited General Psychiatry program prior to applying. External applicants are encouraged to apply. The application process is as follows:
ERAS Common Application which includes:
- Three original letters of recommendation; one of the letters must be from your current training director, the remaining two should be from current faculty you are working with. All letters of recommendation must address your clinical knowledge and skills.
- CV
- Personal Statement
- USMLE or COMLEX Scores (Including Step III, which must be passed prior to the initiation of the Child and Adolescent Fellowship ranking in December)
- Medical School Transcripts
We begin accepting applications in July. Interviews take place on Fridays from September through late October.
There is a match for child and adolescent psychiatry training, with which our program participates. We have six open positions in the match each year. You must register through the National Matching Residency Program (NRMP) in order to finalize your application with us.
For further information, please contact:
Sarah Mohiuddin, M.D.
Director of Child and Adolescent Psychiatry Training
Rachel Upjohn Building
4250 Plymouth Road
Ann Arbor, MI 48109
E-Mail: [email protected]
Residency Coordinator: Karyn Kitchen
Tel: (734) 936-6335
Fax: (734) 936-8907
Email: [email protected]




