Fellowship Overview
The University of Michigan Geriatric Psychiatry Fellowship is a one-year ACGME- accredited program that provides broad-based clinical experience in inpatient, outpatient, long-term care and community settings in an extraordinarily rich academic environment, occurring at the University of Michigan and the VA Ann Arbor Healthcare Systems. Upon completion of the one-year clinical fellowship, the fellow is eligible to sit for the geriatric psychiatry boards.
A two-year fellowship program option (PGY-5 & 6) is available to selected candidates and includes all clinical experience of the one-year program, plus a longitudinal research training component designed to prepare the fellow for an academic career. Our faculty have expertise in health services and policy research, and the fellow can link to extensive resources at Michigan, including the NIH funded Michigan Alzheimer's Disease Research Center, The Institute for Healthcare Policy and Innovation, and the nation’s first comprehensive academic Depression Center, the Eisenberg Family Depression Center. The VA Ann Arbor Health Care System has the Geriatric Research, Educational and Clinical Center (GRECC).
Fellowship Features
- Protected scholarly time (10%), with opportunities for presentation and publication
- Generous individual supervision and mentorship with a large faculty
- Elective rotation opportunities for a customized fellowship
- Conference time, textbook and travel stipend
- Weekly didactic series, including joint lectures with fellows from Geriatrics and CL Psychiatry
- Textbook of Geriatric Psychiatry readings complements the seminar series
- Bi-Monthly Journal Club
- Weekly University and VA Grand Rounds
- Teaching opportunities- Medical Students, Residents, Peers, Interprofessional, Community
- No call responsibilities
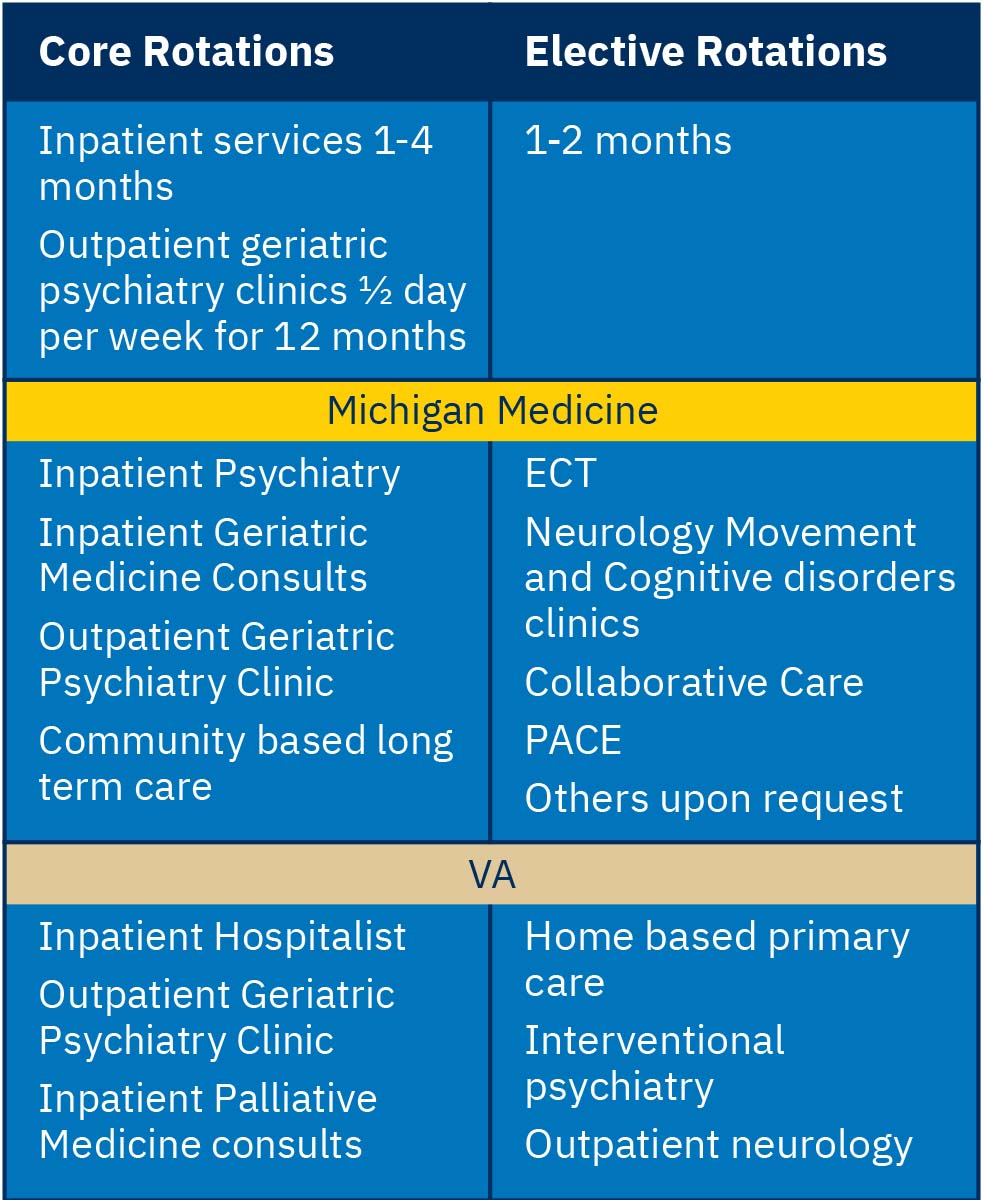
Sample Rotation Schedule:
Program Requirements
Eligible candidates (for either program option) must have:
-
Successfully completed a medical school that is approved by the The Medical Board of California.
-
Successfully completed an ACGME-accredited general residency psychiatry program or a general psychiatry program in Canada accredited by the Royal College of Physicians and Surgeons of Canada.
-
Must be eligible for full medical licensure by the State of Michigan
-
Must have successfully passed USMLE Step III prior to entry into program.
-
Graduates of foreign medical programs must be permanent residents or eligible for a J-1 visa sponsored by ECFMG.
The University of Michigan offers an excellent salary and benefits package from the U-M House Officers Association, a resident run collective bargaining organization.
Why Geriatric Psychiatry?
In geriatric psychiatry, there is no separation between mind and body. There is only a continuum. The patient’s biological, psychological and social issues are all considered when designing tailored clinical interventions. Geriatric psychiatry is among the most “medically-connected” psychiatry specialties. The geriatric psychiatrist never abandons their background in medicine. In addition to biological considerations, geriatric patients benefit by environmental interventions. Geriatric psychiatrists are trained to mobilize systems, including family and community resources to maximize their patient’s functional status.
There is a shortage of geriatric psychiatrists. On a national level, the Institute of Medicine published a report “The Mental Health and Substance Use Workforce for Older Adults: In Whose Hands?” This report calls for bold initiatives and reforms to recruit and retain geriatric specialists to prepare for the health needs of the aging baby boomers. This report signifies a major advance by publicizing the need for geriatric specialists.
Program Director
Sue Maixner, M.D., grew up as the daughter of older parents, with much older grandparents - all four grandparents living within 3 city blocks. As she grew up, she witnessed the interplay of medical events, mobility changes, impacts of hearing and vision loss, life transitions, cognitive changes, financial limitations, and family caregiving. Most importantly, though, was recognizing resilience in her grandparents and parents through their life stories. These experiences ultimately led to a curiosity and passion for geriatric psychiatry - the most challenging field of psychiatry with medical, neurological, cognitive complexity, best provided in interdisciplinary patient and family-centered care settings.
Dr. Maixner earned her M.D. from the University of Nebraska Medical Center, where she developed an interest in Geriatric Psychiatry. At the University of Michigan, she completed her general psychiatry residency and geriatric psychiatry fellowship. She has been on faculty since 1999, and is a Clinical Associate Professor of Psychiatry, Program Director for the Geriatric Psychiatry Fellowship, and Geriatric Psychiatry Program Director at the University of Michigan/Michigan Medicine. Through the American Board of Psychiatry and Neurology, she is board certified in general psychiatry, geriatric psychiatry. As Dr. Maixner’s career has progressed, she cultivated an interest in Hospice and Palliative Medicine (HPM), and also holds this board certification. She is active in the Hospice and Palliative Medicine fellowship, and in the Michigan Alzheimer’s Disease Center’s Rinne Lewy Body Dementia Initiative.
Dr. Maixner’s passion for geriatric psychiatry education extends beyond the clinic. She has a national presence in geriatric psychiatry education. She is a past co-chair of the Geriatric Psychiatry Subspecialty Caucus for the American Association of Directors of Psychiatry Residency Training (AADPRT), and has been a member of the AAGP teaching and training committee for over a decade. In 2014, she was one of five geriatric psychiatrists in the country invited by the ACGME and ABPN to develop the Geriatric Psychiatry Milestones for geriatric psychiatry fellowships. She’s a recipient of the APA’s the Nancy C.A. Roeske Medical Student Teaching Award.







